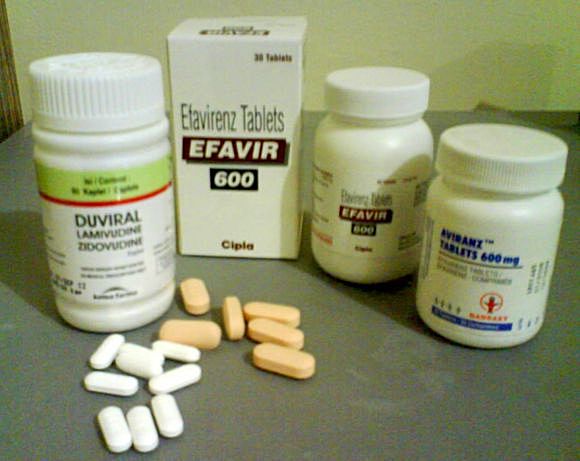
People living with HIV face corruption and incompetence in the health system
Michael Buehler
Nuraini's treatments: precious, but too hard to get |
’Don’t cry! It weakens your immune system!’ This was the first comment made by Dr Irina after she informed Nuraini that her blood test indicated she was HIV positive. Nuraini went to see Dr Irina at a private, up-scale clinic usually frequented by Jakarta’s expatriate community. Nuraini wasn’t especially worried about her health, she had just had a cough for a couple of weeks that would not go away. The HIV positive result was totally unexpected.
Nuraini is a 25 year old, university-educated woman. Born and raised in Jakarta, she worked as a personal assistant in an international company. Nuraini is not her real name. In order to protect her privacy and that of others, pseudonyms have been used for all of the people mentioned in this article.
What Nuraini did not know at the time of her diagnosis was that Dr Irina’s bizarre reaction was just the starting point of a long odyssey through Indonesia’s dismal health system, during which Nuraini would have to suffer through countless meetings with incompetent doctors and become exposed to cynical forms of corruption.
Trying not to cry anymore, Nuraini asked Dr Irina for information about what to do next. ‘You can get HIV from having unprotected sex’, Dr Irina read out loud, hiding behind a big black book. Nuraini had to remind her doctor that she had been diagnosed as having HIV. Therefore, she explained to Dr Irina, she was not so much interested in getting information about how she might contract HIV, but rather wanted to know what to do next.
Dr Irina scribbled the name of Professor Setiawan on a piece of paper and sent Nuraini away. A few days later, it turned out that Dr Irina was more willing to share information, but information of the wrong sort. One of Nuraini’s friends happened to have an appointment at the same clinic. Breaking all the rules of professional confidentiality, Dr Irina informed her other patient about Nuraini’s newly discovered HIV positive status. Nuraini decided to never see the doctor again.
Bad medicine
After several blood tests at other hospitals in Jakarta confirmed the HIV positive diagnosis, Nuraini managed to get an appointment with Professor Setiawan, reputed to be one of Indonesia’s foremost HIV experts. The examination was quick and quiet. Seeing about 60 patients per evening on average, Professor Setiawan spent no more than five minutes checking Nuraini’s blood results and conducting a physical examination. He barely spoke. He did not explain the test results to Nuraini nor did he inform her about what steps she should take next or where she could get additional help.
It was only by consulting websites in internet cafes that Nuraini learned what it meant to have a CD4 value below 200, as her blood test results told her. A CD4 cell count measures the number of CD4 T-cells in each cubic millimetre of blood. A normal count in a HIV negative adult can vary, but is usually between 500 and 1500 cells per cubic millimetre. A CD4 cell count is the main test that doctors use to monitor a HIV positive person’s immune system. If a HIV positive patient’s CD4 cell count falls below 200 cells per cubic millimetre, the person is potentially at risk from certain opportunistic infections, especially pneumonia. Doctors therefore advise people living with HIV and who have a CD4 cell count below this level to start a Cotrimoxazole prophylaxis to prevent such opportunistic infections. Cotrimoxazole is a medicine that has antibacterial effects. It is marketed in Indonesia under the name Bactrim by Roche, a Swiss pharmaceutical company. A locally-produced, generic version of the drug is also available.
These medicines are affordable for most Jakartans. A box of Bactrim, which will last a month, is available in pharmacies around the capital for around Rp200,000, about US$16. Generics are considerably cheaper. Much to Nuraini’s surprise, however, the prescription she received from Professor Setiawan at the hospital did not include Bactrim, but an asthma spray and a box of vitamins, containing pills for two weeks. The price for these two (useless) treatments, which had to be purchased at the hospital, was almost US$100. While the true intentions of Professor Setiawan remain unclear, over-prescribing expensive medicines to uninformed patients is nothing new to observers of Indonesia’s graft-ridden health system. As one executive at a western pharmaceutical company told me: ‘Indonesian pharmaceutical companies have established quite elaborate ‘incentive’ schemes for doctors who prescribe the company’s medication to their patients.’ These incentive schemes include free flights to Singapore for doctors who prescribe certain medicines 500 times or an all-expenses paid trip to Paris for those who write 2000 prescriptions. Doctors sometimes also receive a percentage of the drug price for each prescription they write.
Over-prescribing expensive medicines to uninformed patients is nothing new to observers of Indonesia’s graft-ridden health system
Nuraini refused to buy the vitamin pills during her next visit and informed Professor Setiawan that she only wanted to buy the cheaper but more essential Cotrimoxazole pills. The professor greeted her comment with raised eyebrows. Apparently, he was not used to having well-informed patients. Status counts in Indonesia’s health system, and daring to simply ask a physician why he or she prescribes a certain drug can be interpreted as questioning the doctor’s authority.
Living with HIV
Through a friend, Nuraini learned that some women living with HIV in Jakarta had started to organise themselves. After much hesitation, she decided to attend a meeting of a group called Independent Women (Perempuan Independen) at the Positive House (Rumah Positif) situated in a narrow back-alley in Central Jakarta. Still shocked and sad about her newly discovered condition, Nuraini cried during most of the first meeting she attended in July 2007. But she also listened to the stories of the other women attending.
Unfortunately, those stories were not very encouraging. Soemiati, a 22 year old women and mother of two children, was infected by her husband three years ago. Luckily, her children were negative. Kade, a 45 year old woman from North Sulawesi told the group that after she was told she was HIV positive, her two sisters, both of whom are doctors, forced her to leave the family home. Displaying remarkable ignorance, they apparently feared that a HIV positive person could infect other people in the household. ‘They disinfected the bathroom every time I used the toilet’, Kade told the group. Since then she has only been allowed to see her children every other month through the fence surrounding her family home.
During meetings over the next couple of weeks, Nuraini listened to the women and slowly began to understand what it meant to live with HIV in Jakarta. The way she was treated by the doctors in the hospitals was all too familiar to the women at Rumah Positif. Many of them had been treated in similar ways. Most had also been given prescriptions for long lists of peculiar and unsuitable medications.
It was also during these meetings that Nuraini learned that in certain hospitals it was advisable to use a pseudonym when going for a blood test. Hospital staff had tried to blackmail people living with HIV, threatening to expose their HIV positive status to their families if they did not pay. ‘Who can you trust?’ Nuraini asked during one of these meetings. ‘Nobody but yourself’, one of the women, a former drug addict, replied. Other members of the group nodded their heads. A few days later, Nuraini tried to commit suicide by taking an overdose of sleeping pills.
Starting on treatments
After another suicide attempt a few weeks later and three months of mental agony, Nuraini decided to start Anti-Retroviral (ARV) therapy in October 2007. ARV medicines are used for the treatment of infection by retroviruses such as HIV. They can suppress the replication of HIV and dramatically reduce the amount of the virus in a person’s system, restoring immunity and greatly prolonging life and good health. Theoretically, ARV therapies are free for all Indonesian citizens who need them. International organisations such as the Global Fund finance most of the programs in the country. However, ARV treatments are not freely available in pharmacies. Instead, they have to be collected in special hospitals.
ARV therapies are complicated. They require people living with HIV to take several varieties of medicine a day at the same time each day. Once treatment begins it is vital there are no interruptions to the therapy. If a patient misses too many doses or takes the wrong medication, drug resistance can develop and the virus can begin to replicate again and damage the immune system. If resistance develops, so-called second-line ARV therapies can be started in some cases.
The ARV therapy Nuraini started required her to take three pills a day: one at 8am, one at 8pm and the last one at 10pm. She was told that if she missed more than three pills a month, there was a risk that her body would develop resistance against the ARV therapy and that she might become seriously ill. Nuraini started to ‘train’ by taking vitamin pills first at the necessary hours. Anxious about what the therapy would mean for her health, she took her first ARV pill a few weeks later. Luckily, and unlike some people, she suffered only minor side-effects.
Daily ordeals
Highly motivated, she went back to Professor Setiawan to get a prescription for another month, only to hear that the hospital had run out of pills. She was sent away by the nurse with a small plastic bag containing enough medication for only three days. Reporting back three days later, Nuraini waited for more than five hours, only to be sent away again, this time with no medication at all.
No strangers to such supply shortages, the people at Perempuan Independen had established an informal ‘pill swapping system’. After three days of frantically calling people living with HIV in Jakarta, during which time she constantly thought about what would happen if she ran out of pills, Nuraini managed to get in touch with Wayan, a former drug user living with HIV and Hepatitis C. Even though Wayan only had enough pills for himself for five days, he agreed to ‘lend’ two days worth of pills to Nuraini. Luckily, by the time the two days had passed, the hospital had received new stock. After another seven hours of waiting at the hospital, Nuraini finally received enough medication for two weeks.
Hospital staff try to blackmail people living with HIV, threatening to expose their HIV positive status to their families if they don’t pay
Navigating the bureaucracy of Indonesia’s health system was a constant problem for Nuraini over the following months. She was required to see Professor Setiawan once a month to get a prescription. However, not only was it difficult to get appointments with him, but he often left town for several weeks without notifying his patients. ‘No signature, no pills’, Nuraini learned from the hospital staff. After spending on average a day or two per month trying to get Professor Setiawan’s signature on the prescription, Nuraini usually spent another two days at the hospital trying to get her pills – if the hospital had any, which it often didn’t. Organising her medication became so time-consuming and resulted in so many days of absence from her office that Nuraini came under serious pressure at her workplace.
The distribution of the medication also did not seem to follow a standard procedure. Sometimes, the hospital staff gave Nuraini the ARV pills for free, sometimes they asked her for money. This is illegal since ARV medications are supposed to be free. Once or twice, the staff lost her most recent blood test results or her patient file, leaving her to sit and wait in the hospital for hours . Another time, the pill box she received was full of dead ants.
During a supply shortage in December 2007, the nurses sent Nuraini home with the wrong pills, distributing second-line treatment medication to all first-line patients who showed up that day at the hospital. It was only after Nuraini checked the generic name of the drug on the internet that she found out that the hospital staff had given her the wrong pills. If Nuraini had taken it, she may have developed resistance to the first-line treatment. ‘It is actually not HIV that kills us but the hospital administration’, Ririn, a woman living with HIV in Jakarta, summarised her experience with the Indonesian health system.
The complicity of the development industry
Observing Nuraini’s struggle, some of her friends, including myself, tried to raise the issue with international organisations working on HIV in Indonesia. After all, the fight against AIDS in Indonesia is part of a massive global effort. A lot of the funds for treatments, as well as expertise and strategic planning is provided by international agencies.
I received several late night phone calls from foreign development industry representatives urging me to not talk about supply problems associated with ARV therapies to the media
However, in response to our queries and requests for action, representatives of most organisations responded by pointing to the ‘sensitivity’ of the issue or referring to obscure ‘political interests’ that would not allow their organisations to be more explicit about these obvious problems. I received several late night phone calls from foreign development industry representatives urging me to not talk about supply problems associated with ARV therapies to the media.
Looking for support outside Indonesia, I addressed the issue in several emails with managers of the Global Fund based in Geneva, an organisation which is financing some ARV therapies in Indonesia. One of them responded ‘…we have to be careful before talking about vast corruption or systematic bribery by considering the probably very true story of the person you are mentioning. It does not mean that the whole system is corrupted and accusations must be supported by evidence…I met with the chief executive of [an NGO] two weeks ago in Jakarta…and he never mentioned anything to me related to chronic supply problems of ARVs…’
The fact is that there is a wealth of ‘evidence’ that ‘supports’ the personal experiences of people living with HIV in Jakarta. As the UN recently highlighted in a briefing on the ARV system in Indonesia in August 2008, ‘Supply or distribution problems have dogged the free ARV program since it was launched in 2004. Every three months or so, the country’s largest AIDS e-network, AIDS-Ina, is inundated with complaints over the latest shortages, and the situation seems to be worsening’. There have been countless other media articles about supply shortages all over Indonesia over the last few months.
There is a long list of problems that are widely known but rarely directly addressed by development agencies working on HIV issues: red tape in the health system, corruption in the pharmaceutical industry (for some reason the ARV drugs produced by the Indonesian company Kimia Farma are twice as expensive as the ARV drugs provided by the Clinton Foundation), dysfunction of the supply chain management system, and inaccuracy of the inventory data held by hospital pharmacies to mention only a few.
‘Development workers’ avoid addressing obvious problems not so much because of their ‘sensitivity’, but because one’s career does not prosper if you admit that your program is failing
The reactions of the development organisations I contacted point to larger problems about the modus operandi of the development industry in Indonesia. Complicity between the Indonesian government and the development industry is not unusual in an environment where the careers of foreign ‘development workers’ often depend on the rapid implementation of programs and fast disbursement of funds, rather than on impact analysis. ‘Development workers’ avoid addressing obvious problems not so much because of their ‘sensitivity’, but because one’s career does not prosper if you admit that your program is failing.
No positive news
I would have liked to end this article on a more positive note. But I find it hard to do so, given Nuraini’s ordeals with the health system, and the frustrations of her friends who have tried to take up her case with the development industry in Jakarta.
This 1 December 2008 is the twentieth World AIDS Day. As the official website says, World AIDS Day is ‘important in reminding people that HIV has not gone away, and that there are many things still to be done’. In few places is this message more true than in Indonesia. The Indonesian ARV treatment system is on the brink of collapse. This is not only true for Jakarta, but even more so for centres outside the island of Java. Newspapers in recent months have reported supply shortages in South Sulawesi, Kalimantan and Papua, to name only a few areas.
Kade told the group that once her HIV status was diagnosed, her two sisters, both of whom were doctors, forced her to leave the family house. Displaying remarkable ignorance, they apparently feared that a HIV positive person could infect other people in the household
Meanwhile, the daily stresses caused by the health system and social stigma continue to take a toll on the psychological well-being of people living with HIV. These stresses seem to have been too much for the support group Perempuan Independen. This group, with all the potential for support that it offered, no longer exists. Tuti, one of the women in the group, decided to stop taking ARV because she is no longer able to deal with the daily harassment and incompetence. She now says she is ‘waiting to die’. Nuraini has started to bribe a nurse at the hospital with the equivalent of US$200 a month to make sure she stows away enough pills for her. Soemiati, the HIV positive mother of two mentioned above was unable to afford to bribe hospital staff to ensure a steady supply of ARV medicines. She died as a result of AIDS a couple of weeks ago. ii
Michael Buehler (mb3120@columbia.edu) is a post-doctoral fellow in Modern Southeast Asian Studies at the Weatherhead East Asian Institute at Columbia University in New York.