An Indonesian medical doctor reflects on rural health practices
Brahmaputra Marjadi
Incorrect processing methods render instruments non-sterileBrahmaputra Marjadi |
In a rural district in Indonesia, a 30-something year old man received an intravenous antimalarial treatment after a laboratory test came back positive for malaria. The diagnosis was unremarkable in an area where malaria affects more than 75 per cent of the population. What was surprising was how the disease came to be diagnosed. Most people know that malaria is caused by a blood parasite spread by mosquitoes. But this particular case was caused by a buffalo.
The man had been riding his motorbike around midnight with no headlight and no helmet when he hit a buffalo. He was taken to the hospital and admitted with a mild head injury. So how did this textbook-case traffic accident lead to malaria? Although the patient had no indication of the spiking fever, chills, pains or profuse sweating associated with the acute phase of the disease, his blood was tested for malaria. When I asked the attending physician why he requested the test, he laughed and said, ‘There was actually no indication for the malaria test. We are just so used to circling the malaria option in the laboratory request form that we do it indiscriminately.’
As I discovered, this was not an isolated incident. Many other patients had been subjected to malaria testing regardless of their clinical presentation. I also found malaria diagnoses among patients who were admitted with unrelated conditions such as chickenpox, ear infections and appendicitis. Two physicians jokingly called these cases ‘malaria laboratoris’ (laboratory malaria) because the malaria diagnosis was based solely on the results of a laboratory test.
A dangerous practice
The doctors consider ‘malaria laboratoris’ to be a mere harmless oddity. But its consequences are potentially severe. In this isolated region, a diagnosis of malaria in a hospitalised patient triggers a treatment regime that invariably includes intravenous antimalarials – drugs which have many side effects and should only be reserved for patients who cannot take medication orally. The risks from intravenous therapy occur everywhere, but they are even more serious in poor, isolated areas, where a strong desire not to waste resources can lead to risky practices. In this district, intravenous catheters and syringes and needles used to inject drugs into intravenous lines are reprocessed for multiple usage using faulty sterilisation protocols. Leftover infusion fluids are often re-used for other patients after being stored for several days without refrigeration. In Indonesia’s hot tropical climate it only takes a few hours for bacteria to grow in the fluid. The combination of these contaminated syringes, needles and fluids is very likely to cause serious infections in patients’ bloodstreams.
Many patients are subjected to an unnecessary high risk of bloodstream infection in an attempt to treat a disease that they never actually had
These kinds of risks may be the lesser of two evils in cases where missing out on an infusion could lead to a patient dying. But in this district many patients did not need the intravenous therapy in the first place. An audit by a malaria expert revealed that most malaria test results had been incorrectly interpreted. So not only are patients tested unnecessarily, but their test results are often wrong. Consequently, many patients are subjected to an unnecessary high risk of bloodstream infection in an attempt to treat a disease that they never actually had. Even if the patients indeed have malaria, their clinical conditions often still allowed them to take the much safer oral drugs. Why, then, the widespread practice of high-risk intravenous therapy, one might ask?
The non-clinical culprits
An intricate web of beliefs is responsible for these kinds of dangerous clinical practices. Patients believe that intravenous medications are the most effective drugs available, and demand that they get them. Doctors and nurses administer intravenous therapy despite the lack of medical indications to meet this demand. As one doctor explained, ‘My patients keep complaining when they are given oral drugs, but once I give them intravenous drugs, they stop complaining instantly.’ In this district, the cultural concept of being hospitalised is incomplete without receiving an intravenous therapy. This belief has also infiltrated the health workers, who admitted to feeling as if they were ‘doing nothing for the hospitalised patients’ if they did not prescribe it.
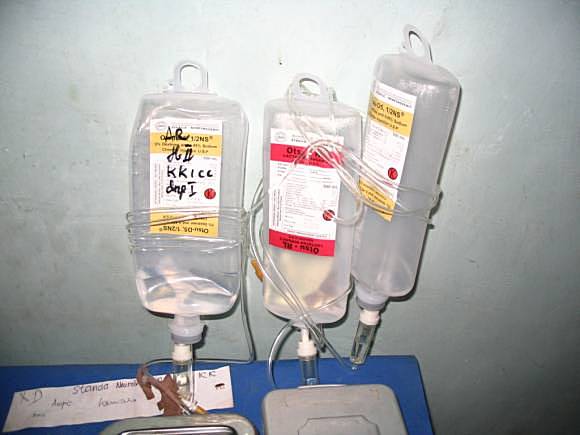 |
Leftover infusion fluid containing antimalarials saved for use in other patientsBrahmaputra Marjadi |
Although the danger for patient safety from sub-optimal clinical care seems obvious, limited laboratory facilities make it virtually impossible to detect. Doctors and nurses argue that healthcare-associated infections do not exist among their patients because they have never seen any proof that they do. This belief has led to a dismissive attitude towards infection risks. A senior nurse told me, when asked about the use of non-sterile instruments, ‘You see, Doctor, when we try to do our best, God knows and He doesn’t allow bad things to happen, even when the instruments are not sterile.’ These attitudes are shared by health service managers who did not consider infection control as a high priority for resource allocation.
A long way to go
Improving infection control and patient safety in rural Indonesia is a great challenge. The main challenge is not lack of facilities, because various donors have helped in this regard. Rather, it is health workers’ lack of knowledge. The majority of rural nurses still come from nursing high schools where they study a curriculum inadequate for their job. Many junior doctors do not have access to up-to-date literature during their training and therefore tend to adopt practices of senior clinicians without question.
The few health workers who learn and try to implement scientifically proven practices face enormous pressure from patients, colleagues and management to abandon these for the status quo
The situation is made worse by a lack of motivation among health service managers. The fee-for-service, out-of-pocket payment of healthcare expenditure means that patients, not hospitals, pay the extra costs of healthcare-associated infections. When a patient develops an infection, they need more laboratory tests and sophisticated antibiotics, and longer hospital stays – services which actually increase hospitals’ revenues. Patients and health workers in rural Indonesia are unlikely to challenge these policies because they think they are lucky to have any health services at all.
But perhaps the biggest challenge is shared cultural beliefs. Weaknesses in medical and nursing training mean that patients’ beliefs concerning intravenous therapy or antibiotics remain unchallenged. Before becoming clinicians, health workers spend almost two decades immersed in these beliefs. The few health workers who learn and try to implement scientifically-proven practices face enormous pressure from patients, colleagues and management to abandon these for the status quo.
Clearly, a collaborative effort is required to solve these problems. Only concerted actions from clinicians, public health professionals, educational institutions, professional organisations and the government can tease out the complex challenges of patient safety in rural Indonesia. There is a long way to go, but this is the only chance we have to prevent more people from becoming victims of buffalo-induced malaria. ii
Brahmaputra Marjadi (b.marjadi@gmail.com) is an Indonesian medical doctor and lecturer who has just completed his PhD in public health at the University of New South Wales.











