As infectious diseases spread, strategic governance becomes ever more important
Scott Naysmith
Indonesia is struggling to manage the burden of infectious diseases. In parts of Java there is a resurgence of diphtheria in children, stemming in large part from parents’ resistance to vaccinating their children. Public health officials across the archipelago are finding a greater than expected prevalence of lymphatic filariasis, commonly known as elephantiasis. Polio, once believed eradicated from the country, was reintroduced around 2005 by returning pilgrims infected while performing the haj in Mecca. Avian influenza has infected and killed more people in Indonesia than in any other country. These and other communicable diseases not only cause great suffering for those infected, but they also negatively impact on social and economic development and will increasingly compound the effects of non-communicable diseases, such as diabetes.
Controlling infectious diseases hinges upon a government’s ability to implement effective interventions. Since independence, Indonesia has experienced drastically different forms of government, ranging from centralised authoritarianism to decentralised multi-party democracy, each bringing unique constraints and opportunities to the task of containing infectious diseases. Whereas Suharto was able to employ coercive strategies for containing disease, the decentralised structure of government in contemporary Indonesia needs to pay more attention to providing incentives to local populations so that they participate in and comply with disease control programs.
Authoritarian responses to disease
In 1966, when the World Health Organization (WHO) formulated the global strategy for the intensified Smallpox Eradication Program, Indonesia was the second worst affected country after India. Smallpox programming was plagued by significant financial and logistical challenges. Historically, smallpox eradication was underfunded by the government and the international community. There was also a dearth of infrastructure and limited public health capacity to support vaccination and disease surveillance and reporting. Moreover, some parents believed that the vaccine harmed more than helped and consequently resisted vaccination for their children. And then there was the burden of geography: as one WHO observer noted in 1974, all you had to do was look at a map of Indonesia to realise the challenge of eradicating smallpox from every corner of the sprawling archipelago.
Despite these many barriers, doctors diagnosed the last case of smallpox in Indonesia in 1972 and then declared the country smallpox-free after a period of 18 months with no new infections. What accounts for the program’s success in the face of such serious challenges?
There are many factors that led to the eradication of smallpox in Indonesia, but a fundamental feature of the program was the commitment and strong-arm tactics exercised by Suharto’s New Order government. The New Order government understood that eradication would be successful only when every last case had been identified and contained. Through central government decree, Jakarta implemented an unwavering campaign, using soft coercive practices to ensure people complied with programming. The government employed all elements of the security forces, including the police, national armed forces, and hansip (local defense forces) to track unvaccinated persons, enforce quarantine and vaccination, and ensure cases were reported to government officials. Participation in smallpox eradication was not optional and there was little space for individuals or local authorities to resist or avoid the program. Later, the WHO pointed to Indonesia’s successful eradication of the virus as a positive example in the difficult final years of eradication programming in India and Bangladesh.
Decentralisation and disease
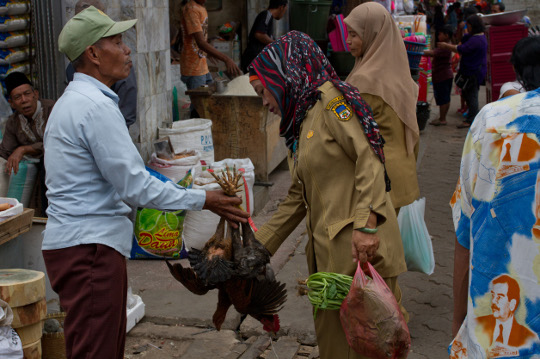
Shoppers handling live birds in a market in Lampung - Scott Naysmith
After Suharto’s government collapsed in 1998, Indonesia underwent a drastic and rapid reordering of political authority. Guided by international institutions like the World Bank and the International Monetary Fund, Jakarta relinquished much of the responsibility for health services to district level administrations. The results have been mixed.
To an extent, decentralisation has promoted local ownership of health priorities and created opportunities for tailor-made interventions suited to local contexts. At the same time, decentralisation has weakened rural health structures and created disincentives for preventative public health. With local officials now allocating funding and setting priorities, infectious disease containment has become more difficult. Infectious diseases are apolitical: such pathogens do not recognise political boundaries and readily travel on the backs of birds and in the lungs of people as they cross the country. As a result, controlling infectious diseases demands coordination at every level of government – a requirement at odds with the decentralised structure that currently defines Indonesian politics.
Nowhere is this more apparent than in recent attempts to contain avian influenza, commonly known as bird flu or the H5N1 virus. Live birds host H5N1 and since 2003 the virus has been found in every province. People who live and work intimately with poultry are considered the most at-risk for becoming infected – a particular problem considering that most Indonesians raise birds at home. The mortality rate for Indonesians infected with H5N1 is, incredibly, above 80 per cent.
Controlling the spread of the virus is difficult as millions of birds travel from farms to markets across district and provincial borders, loaded on trucks and along the sides of motorbikes, every day. Though some district officials actively seek and test poultry for avian influenza, such activities can be rendered null by both the movement of poultry and when neighbouring officials fail to take similar precautions.
Government officials are rarely aware of programming or disease outbreaks in nearby provinces. Aceh, for example, imports the vast majority of birds from Medan, a hub of commercial poultry farming that has experienced repeated outbreaks of avian influenza in both commercial and backyard poultry stocks. Yet Acehnese officials in charge of animal health in districts receiving thousands of birds a week from Medan have never met with their counterparts in North Sumatra. Such knowledge sharing is crucial to contain the disease.
Incentives not enforcement
The main strategy for containing avian influenza is depopulation – culling – of suspected infected poultry. This requires encouraging bird owners to report suspected infection in their flocks and then watch as their birds are killed. District and provincial governments have been inconsistent in their application of this tactic since 2003. Compensation for culled birds is extremely rare, and if money is disbursed it is paid at below market value. Some bird owners have taken to hiding their flocks from government officials to avoid loss of livelihood. Many farmers in Aceh, Banten, and Lampung report that they sell their birds promptly at the first sign of sickness. In short, there is both an inability to enforce culling coherently and insufficient compensation to encourage wide-scale reporting of sick poultry.
In the absence of a strong centralised system to track, report, and enforce disease control programs, all levels of government – central, provincial, and district – must ask what levers of political power exist to contain infectious diseases that readily spill across provincial and district borders?
While top-down methods preferred by the New Order government are relegated to history, the central government still has a significant role to play in containing infectious diseases. Jakarta must support the provinces and districts with financial and political commitments, and assist in brokering interventions sponsored by bilateral and multilateral donors. Provincial and district governments must commit financial and human resources to long-term programming extending beyond the tenure of their elected officials. The central government can and should provide a forum for better cooperation across political boundaries. Ultimately, however, understanding what economic and social incentives exist for local populations to participate in and comply with infectious disease control programs will determine the success of these interventions in decentralised Indonesia.
Scott Naysmith (scottnaysmith@gmail.com) is a doctoral candidate in the Social Policy Department at the London School of Economics and Political Science and a Trudeau Doctoral Scholar, supported by the Pierre Elliott Trudeau Foundation.











