HIV-related stigma and is making access to healthcare during the pandemic difficult
Najmah, Kusnan & Sharyn Graham Davies
“I prefer to treat COVID-19 patients (rather) than HIV-patients.”
It is difficult to imagine a health care worker saying this to a patient, but it is evidence of the stigma that continues to surround HIV-patients in Indonesia.
Imagine if a pregnant mother delivered a baby, suffering not only a painful birth but also a broken heart due to the way she was treated by health service workers. Infected with HIV through unsterile medical equipment, she has had to bear the stigma of being branded an ‘irresponsible’ mother. This article draws attention to the unfair treatment and disrespect health service providers have shown HIV-positive mothers during the first year of the COVID-19 pandemic in Palembang, South Sumatra.
HIV-related stigma is still rampant in Indonesia. Stigma, according to Goffman, is 'an illuminating excursion into the situation of persons who are unable to conform to standards that society calls normal'. Parker and Aggleton argue that understanding stigma requires consideration of the intersectional influences of the broader social, cultural, and economic factors that structure stigma beyond the level of the individuals. We define HIV-related stigma as negative beliefs, feelings and attitudes towards people living with HIV and their families; for people who work with HIV service providers; for members of high-risk groups such as Intravenous Drug Users (IDUs), female sex workers, men who have sex with men; and for married women living with HIV.
During the first year of the COVID-19 pandemic, for women living with HIV who sought health services during delivery or therapy for other diseases, our research in the city of Palembang, South Sumatra, has found that the stigma attached to HIV extended to personal and community judgement related to COVID-19. Below we share some of the stories we heard.
Yana’s story
In October 2020, Yana*, 25 years old, was rushed to hospital to deliver her fourth baby. Based on her previous experiences, she knew she needed to access Prevention Mother-to-Child of HIV transmission (PMTCT) services at one public hospital in Palembang. Yana was aware she needed to disclose her HIV status in order to protect health workers and so her baby could get prophylaxis therapy after her delivery.
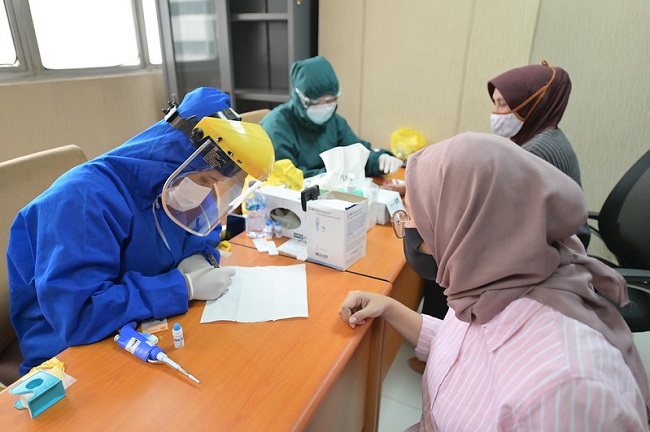
Yana was treated in the emergency room and was asked questions related to COVID-19 symptoms for screening purposes. The health workers treated her well until she disclosed her HIV status. After she disclosed her HIV status, the nurse pushed her body and said, “Why didn’t you tell us earlier?” A midwife added, “I prefer to treat COVID-19 patients (rather) than HIV-patients.” Another health worker said to her:
“If you were tested for COVID-19, the result is more likely positive. I said, no, I am not COVID-19 positive. I am healthy…if I get infected with COVID-19, you would be sick too. Then the health worker was silent.”
Then, Yana exercised her rights and replied:
“I have the right. I can make a report about your unfair treatment of me. Please don’t treat me badly. For my HIV status, it is not my own willingness, as I also did not want to be infected with HIV. My operation schedule failed as the date of prediction was on 15th December 2020. The health workers keep talking though I was bleeding and in pain. My heart was broken. Help me, God.”
After her complaint, another doctor helped Yana. The doctor expressed the importance for the HIV-positive mother to exercise her sexual and reproductive rights in order to access respectful treatment and get the support of health workers for HIV-positive women, particularly during her delivery. The doctor highlighted that HIV-related stigma never vanishes, and consequently HIV-positive women and their husbands need to be resilient for the sake of their child’s health. She felt better after her uterus (womb) was cleaned properly and expressed her gratitude to the second doctor.
“Then another doctor helps me, and said to one midwife who treated her ‘if you cannot finish your work to help this mother, it is better not to treat her delivery’. The unprofessional treatment for HIV-positive pregnant women would kill the mother and baby, the doctor added.”
Yana and her husband are among the rare groups living with HIV in Indonesia who dare to speak up and argue with health workers. It is an unfortunate reality that the lack of professionalism of health workers and the stigmatisation of HIV patients are still problems that cannot be overcome. As we can see from Yana's story, it is necessary to have a brave and confident voice like hers. Of course, the number of those who can do this remains very small, as most people choose to remain silent because they are powerless.
Listen to Yana's story as she told it, via YouTube
Nika’s story
In July 2020, 33-year-old Nika* suffered from appendicitis and needed to undergo surgery. She decided not to disclose her HIV status so that she would get respectful health treatment. Nika believes that the HIV-related stigma has become worse during the pandemic. Based on her experience, every patient was suspected of having COVID-19 during the first year of the pandemic, and disclosure of HIV status meant a double burden of stigma for HIV-positive women in health settings. She recounts that:
"[In July 2020] Yes, I seek health services in a hospital, I do not disclose my HIV status. There is the strong stigma of being an HIV-positive mother, I cannot imagine if I disclose my HIV status. I really do not want to open my HIV status. You know why? I access the third class facilities (there are 5-8 patients in a room), and stigma is strong during the COVID-19 pandemic (every patient was suspected of having the virus). I am alone during my hospitalisation, no companion (from family) was allowed. If I am open about my HIV status, people will not treat me (run from me), no one will take care of me, inject the medicine for me. In my observation, health workers are still afraid of HIV compared to COVID-19."
In February 2021, Nika was sick again and she went in a rush to the emergency hospital with her mother. She was coughing and had difficulty in breathing. She was directly diagnosed with COVID-19 and was treated in an isolation room for 10 days although a few days later her result showed negative for the virus. Nika expressed:
“I needed to wait for three hours to get treatment in the emergency room. Due to my symptoms related to COVID-19, frequent coughing and difficult to breathe, I was treated in an isolation room directly. Well, I got the benefit I did not need to share with another patient who may be COVID-19 positive. A robot, the name is Raisa, also helps to provide medicines for me, nurses will visit us only at a certain time.”

Lessons to learn
HIV-positive women are aware that every woman may deal with different stages of stigma from family, health workers, friends and neighbours. Therefore, they need to consider to whom they need to disclose their HIV status. During the pandemic, HIV-positive women need to be brave enough to seek health services while most people may avoid accessing the hospitals. The prospect of every patient being diagnosed with COVID-19 was rampant in the community in the first ten months of the pandemic. We argue that the women may lose either way, through disclosing or not disclosing their HIV status in a health setting. Therefore, HIV-positive women need to be resilient, drawing on support from their family, supportive health workers to access health services for the sake of their children’s and their own health.
The government needs to create supportive health systems, including peer education for health workers who are able to provide safety and confidentiality for HIV-positive women. In this way, the women feel safe, protected and appreciated as good and religious mothers and wives to reduce the institutionalised stigma in society. In this context, we suggest that the Ministry of Health, in collaboration with the Ministry of Education, needs to include sexual and reproductive health rights and gender equality, particularly for HIV-positive women in the health curriculum.
*Names have been changed for privacy reasons
Najmah (najmah@fkm.unsri.ac.id) Department of Epidemiology, Faculty of Public Health, Sriwijaya University; Kusnan, Postgraduate student in School of Graduates and Professional studies, INCEIF, Malaysia; Sharyn Graham Davies (sharyn.davies@aut.ac.nz) Director of the Herb Feith Indonesia Engagement Centre, Monash University.
This research is funded by Alumni Grant Scheme Round 2 for Indonesia (Australian Awards in Indonesia).
